Navigating the Storm: How Black and South Asian Parents Really Decide on Childhood Vaccines
 Featured
Featured
- Research
- 9th January, 2026
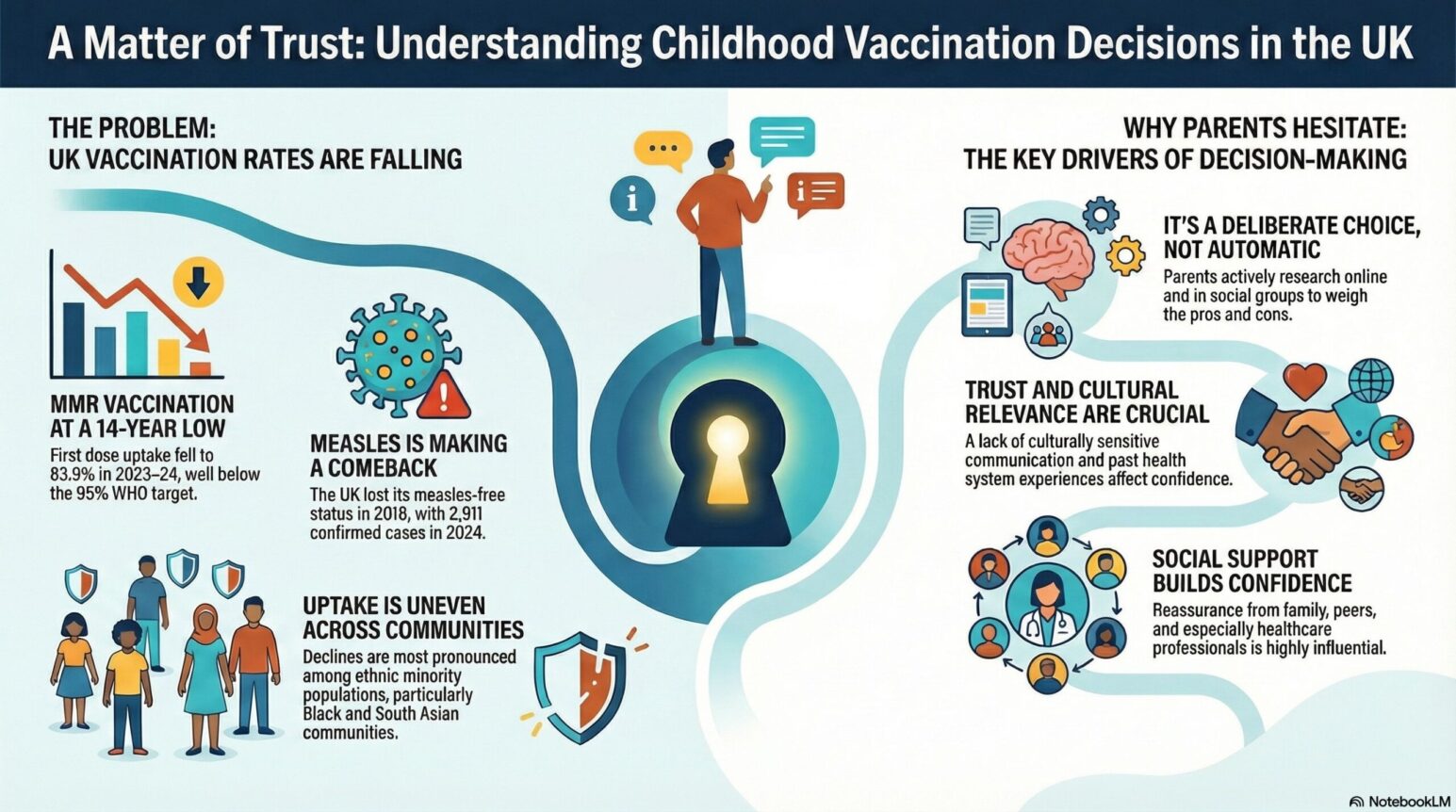
Childhood immunisations are one of public health’s greatest success stories. Yet, in recent years, vaccination rates in the UK have slipped below the levels needed to keep everyone safe—particularly within Black and South Asian communities.
Why is this happening? Is it simply a lack of information? Or is something deeper at play?
Our latest study invited 17 parents from Black and South Asian backgrounds to share their experiences. What we found challenges the idea that vaccine hesitancy is just about a “knowledge deficit.” Instead, for these parents, vaccination is a complex, negotiated process fueled by care, responsibility, and the need for trust.
Here is what we learned about how these parents navigate the system.
The Big Picture: A Decision-Making Map
Our research uncovered three main themes that drive the decision-making process. It is not a straight line from receiving a letter to getting the jab; it is a journey involving research, cultural factors, and emotional support.
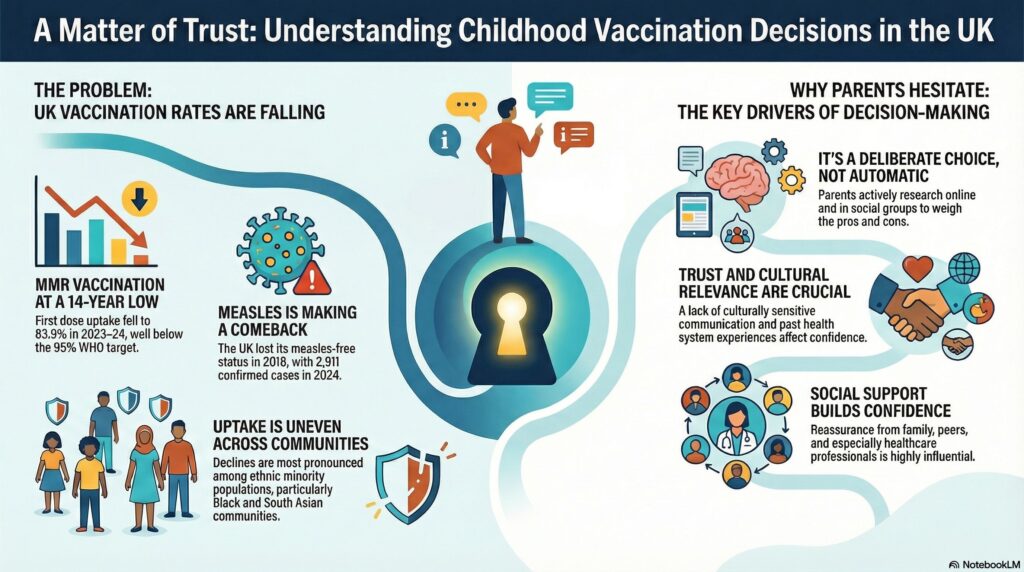
A thematic map showing the three pillars of vaccination decision-making: Weighing Pros/Cons, Systemic Fit, and Weathering the Storm.)
1. It’s Not Automatic: Weighing the Pros and Cons
For many parents in our study, the decision to vaccinate wasn’t automatic—it was a “deliberative and negotiated process”.
Parents didn’t just accept the appointment letter; they actively sought to fill “information gaps.” Many turned to web searches, online chat groups, and community forums to verify claims and clarify doubts before discussing them with their partners.
One participant described watching a documentary about autism risks and then searching for research papers to prove or disprove the claim before feeling safe to proceed. This proves that hesitancy often stems from a place of deep protectiveness over their child’s well-being, rather than indifference.
2. One Size “Doesn’t Fit All”
While parents praised the NHS for effective appointment logistics (the “when” and “where”), many felt the system failed to address the “why” in a way that resonated with their communities.
♣The Information Gap: Standard leaflets often felt insufficient. Parents expressed a need for detailed, culturally adapted information that specifically addressed fears about side effects.
♣The Trust Factor: Trust was the cross-cutting theme. While some parents felt reassured by nurses who explained the process clearly, others felt that historical mistrust and a lack of open dialogue eroded their confidence.
As one parent noted, generic advice isn’t enough: “There are a lot of parents, especially from my culture that don’t want their children to get vaccinated because they’re scared of the side effects”.
3. “Like a Storm Coming”
Perhaps the most powerful insight was the emotional weight of the process. Parents described the vaccination period as a “storm”.
They knew the storm would pass, especially if they had “weathered” it before with older children. But for new parents, surviving this storm required a strong support system. The presence of partners, mothers, and supportive healthcare staff acted as a protective shield, helping them get through the appointment.
How Can We Improve?
The parents in our study offered clear recommendations on how the healthcare system can better support them:
♦Modernise Communication: Move beyond simple leaflets. Parents suggested using QR codes that link to detailed videos or updated digital documents.
♦Create Safe Spaces: There is a desire for group settings or workshops where parents can have “open-minded conversations” to dispel myths and ask questions without judgment.
♦Cultural Sensitivity: Healthcare providers need training to offer respectful, detailed explanations that address specific community fears rather than dismissing them.
The Takeaway
Vaccine hesitancy in Black and South Asian communities is not about rejection; it is about negotiation. It is a process shaped by emotion, culture, and a desire to protect the child.
To rebuild trust and improve uptake, we must move away from a “one size fits all” approach and start navigating the storm alongside parents—with transparency, empathy, and respect.
Author: Dr Glory Aigbedion (Public Health Researcher & Consultant)

 Share Post
Share Post

